 |
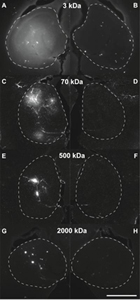
| The diffusion of dextran molecules into the brain with an open blood barrier (on left), compared to one where the barrier is intact (on right).--Courtesy of Elisa Konofagou |
Columbia University scientists showed that it is possible to control the size of the blood-brain barrier (BBB) opening by varying the pressure of an ultrasound beam, a discovery that could herald major breakthroughs in the treatment of neurological diseases.
"This is an important breakthrough in getting drugs delivered to specific parts of the brain precisely, noninvasively, and safely, and may help in the treatment of central nervous system diseases like Parkinson's and Alzheimer's," said Columbia University biomedical engineering professor Elisa Konofagou in a university news release.
"We know that Parkinson's disease would benefit by delivery of therapeutic molecules to the neurons so as to impede their slow death. But because of the virtually impermeable barrier, these drugs can only reach the brain through direct injection and that requires anesthesia and drilling the skull while also increasing the risk of infection and limiting the number of sites of injection. And transcranial injections rarely work--only about one in 10 is successful," she continued.
Konofagou and her Columbia colleague Hong Chen of the Department of Radiology added a wrinkle to the current BBB delivery paradigm by varying the pressure of the focused ultrasound beam that aids the microbubble in crossing the barrier. The team found that smaller molecules were able to penetrate the barrier at lower acoustic pressures and bigger ones at higher pressures; almost all of the previous studies on this topic have focused on one specific-sized agent that is used as an ultrasound contrast agent, says the news release.
The two scientists tested the delivery system by delivering different-sized sugar molecules (dextran). More details are available in an article in the Journal of Cerebral Blood Flow & Metabolism.
"Through this study, we've been able to show, for the first time, that we can control the BBB opening size through the use of acoustic pressure," Konofagou said in the news release. "We've also learned much more about the physical mechanisms associated with the trans-BBB delivery of different-sized agents, and understanding the BBB mechanisms will help us to develop agent size-specific focused ultrasound treatment protocols."
Konofagou's National Institutes of Health research grant was recently renewed for four years and $2.22 million. She hopes to test the delivery method in clinical trials within 5 years, Columbia said in the release.
Not surprisingly, the body protects the brain from foreign substances (including beneficial drugs) quite effectively, and the BBB has proven to be a tough challenge for drug delivery. In another recent breakthrough, Mayo Clinic scientists injected the synthetic peptide K16ApoE intravenously into mice. The peptide binds to proteins in the blood, the combination of which is recognized by receptors on the BBB and allows for its natural, passive transport into the brain.
- read the news release
- here's the study abstract