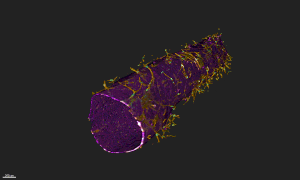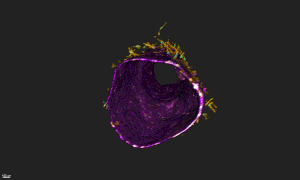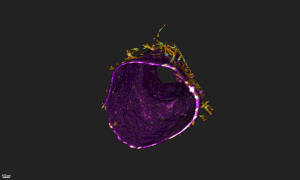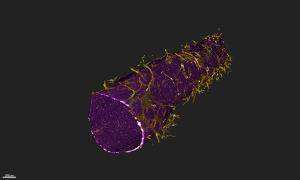
Harvard's blood-brain-barrier-on-a-chip--Courtesy of Harvard
A Harvard University team touted its blood-brain-barrier-on-a-chip, demonstrating the drug delivery applications of the emerging technique to test molecular candidates in vitro by creating miniaturized models of human anatomy.
Researchers at Harvard's Wyss Institute used a microengineering technique to fabricate a hollow blood vessel lined with human endothelial cells and surrounded by an extracellular matrix similar to that which exists in people. The result is a model of the human blood-brain barrier that can be used to study new drug delivery techniques for attempts to surmount a biological barrier that has so far proven largely impenetrable and has been the death knell of candidates for diseases such as Alzheimer's.
"The blood-brain barrier is the first line of defense against chemicals and molecules that could induce brain injury, but it also blocks transport of potentially life-saving therapeutics to the central nervous system," said Wyss Institute Founding Director Donald Ingber in a university release.
The breakthrough comes as the shortcomings of animal models become apparent. The physical and chemical barriers to drug delivery are often different in various species, making mice and other animals imperfect predictors of success in humans, according to an article in the National Institutes of Health's cancer nanotechnology roadmap by Purdue University researchers. They said new in vitro tests that imitate the insides of the human body are needed.
The Harvard team said its blood-brain-barrier-on-a-chip device is more sophisticated than traditional in vitro cell culture techniques that do not emulate important 3-D structures in the body.
Intriguingly, the blood-brain-barrier-on-a-chip component demonstrated self-assembling behavior, meaning it automatically oriented itself in a permutation similar to what's seen in vivo when put in the same environment.