 |
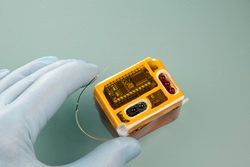
| A wearable drug delivery device designed to treat hearing loss--Courtesy of Draper Lab |
Which organ is so small and inaccessible that surgery there is impossible? It's the inner ear, says Stanford University School of Medicine hearing specialist Robert Jackler.
The millimeters-wide opening has long stymied efforts at drug delivery as well, but, as of late, progress is being made, according to Scientific American.
"We've tried directed medication when treating hearing disorders but the way we do it today is very imprecise and poorly calibrated," Jackler said in the article.
The nonprofit Draper Laboratory in Cambridge, MA, is making progress in creating a small intracochlear device designed to treat hearing loss, according to a February study in the journal Lab on a Chip, as published last month in FierceDrugDelivery.
In a related ear drug delivery initiative, its researchers are also developing a specialized polymer for intracochlear delivery in collaboration with the Pentagon and MIT scientist Robert Langer. The project was initiated in 2012, when the Department of Defense commissioned a project to find a treatment for tinnitus, or ringing in the ears, a problem affecting more than 40% of all veterans.
With the help of MIT's Langer Laboratory, the Draper team is working to create a trigger mechanism for the drugs using wireless remote control and other means.
"The classic problem is how (to) get a local delivery source that distributes over a long period of time," Draper biomedical engineer Jeffrey Borenstein told Scientific American. "We want our device to be able to treat a problem for months if needed."
Meanwhile, the goal of the federally funded project to create an intracochlear drug delivery device is to deliver medication that treats damaged sensory hair cells in the inner ear known as stereocilia. The death of those cells can lead to permanent hearing loss.
Borenstein and colleagues have created and tested a prototype pump on guinea pigs, according to a paper in the journal Biomedical Microdevices. Drug delivery challenges include ensuring a sufficient quantity of the drug enters the ear at a fast enough rate, but putting too much fluid in the inner ear leads to damage, says Scientific American.
How much is too much? More than a drop. Given the size of the inner ear, it's not surprising that another challenge is making the micropump truly micro so that it can fit behind the ear, in a space of about 7 or 8 cubic centimeters, according to Scientific American.
It would work by withdrawing inner ear fluid, adding the medication to the fluid, and then reinserting the fluid in the inner ear. But the delivery system cannot increase the fluid's volume. In addition, the team wants to make the pump implantable, instead of head-mounted, as is the case right now.
Creating a functional intracochlear drug delivery system, whether in the form of a device or a polymer, is critical to the success of efforts organization like GeneVec and Novartis ($NVS), who are collaborating on a gene therapy project to regrow the inner ear's hair cells.
- here's the article in Scientific American
- read more in the paper abstract